Table of Contents
Arthritis is a form of inflammatory disease, acute or chronic, which affects the joints. Depending on its extension, arthritis can be mono arthritis, when one joint is affected; oligoarthritis, inflammation of two to four joints; and polyarthritis, inflammation of five or more joints.
Arthritis is most often initiated by an abnormal friction of fibers of a tendon (flexible but fibrous connective tissue that connects muscle to bone) abnormally applied on a bone or a joint. Arthritis can also occur following a trauma or an infection. Sometimes, the disease results from a complication of an autoimmune disease in which the body attacks its own tissues. In some patients, however, no cause is found to explain the development of arthritis. Regardless the cause, arthritis is always characterized by pain, stiffness and swelling in one or more joints.
Arthritis is very common throughout the world. It is estimated that about one adult in six suffers from some form of arthritis.
Arthritis Symptoms
Arthritis symptoms vary depending of the organ affected. Therefore, some patients can complain of gland swelling (mostly in migratory arthritis), fever, appetite loss, fatigue (due to lack sleep). In some patients, arthritis can affect the functioning of certain organ including but not limited to lungs, heart, or kidneys.
Chronic arthritis can be characterized by a so severe pain that it can awaken or prevent you from falling sleep. The epidermis of the affected area becomes pink, red or purple. The inflamed joints are warm and painful. In some circumstances, Tenderness of the inflamed joint can occur.
Arthritis Causes and Risk Factors
The causes of arthritis differ from one type to another. There are over 100 types of arthritis grouped in four main categories: aseptic inflammatory arthritis, also called inflammatory arthritis, is the most common category; Septic arthritis, which is caused mostly by infection; arthropathy (arthritis), a rare form of arthritis caused by some nervous system diseases; and microcrystalline arthritis, which is due to presence of a bacterium and micro-crystals in the joints.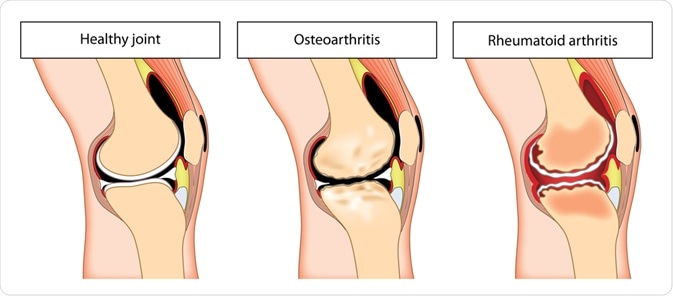
Inflammatory arthritis – form a group of disease caused by different factors
- Rheumatic fever – is a type of autoimmune inflammatory disease that affects few joints, primarily knees and ankles. The inflammation is very painful, but does not last. If left untreated, it can affect the heart and possibly the brain.
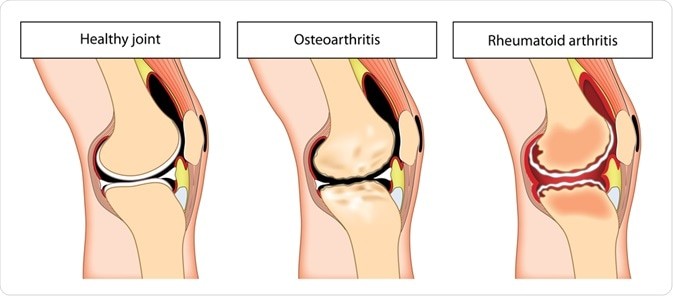
- Rheumatoid arthritis belongs to the group of autoimmune disease, is the most common inflammatory rheumatism. The cause of the disease is not well known; however, researchers suggest overwork, infection and weakened immune system can increase the risk of its development. It affects several joints simultaneously, especially the fingers and wrists. Rheumatoid arthritis is a chronic illness; its symptoms can persist for years.
- Reactive arthritis (ReA) is chronic form of arthritis that occurs in response to enterobacteria infection. This type of infection, located outside of the joints, is mainly caused by urinary tract infection, gastrointestinal infection or genital infection.
Reactive arthritis was first described in 1916 by a German military physician, Hans Reiter. However, it is in 1973 Scientists have discovered that the disease is especially triggered in carriers of a hereditary leukocyte group (Human Leukocyte Antigen B*27 or Group HLA B27) also present in 90% of subjects suffering from ankylosing spondylitis.
- Ankylosing spondylitis, also called Spondyloarthritis , is a chronic inflammation of the spine and the sacroiliac joints. The inflammation is very painful and can last for years. The disease can lead to ankylosis, complete or partial rigidity of the joint. Over the years, Ankylosis can lead to loss of mobility of the spine. Ankylosing spondylitis is more common among men than in women.
- Psoriatic arthritis, also called Psoriatic arthropathy, is a type of inflammatory arthritis associated with psoriasis. It is very common in those who have the Human Leukocyte Antigen B*27 (Group HLA B27). Psoriatic arthritis can affects people at any age; however, it is more frequent in those between the ages of 30 and 50. Unlike Ankylosing spondylitis, this disease equally affects men and women.
- Juvenile chronic polyarthritis, or Still’s disease, is a chronic disease resulting in joint pain and inflammation that mostly affects children under 4 years. It is a symmetrical polyarthritis (or simply symmetrical arthritis) associated with swollen lymph glands (adenopathy), enlarged spleen (splenomegaly) and a rash.
Septic Arthritis: also called infectious arthritis, this type of arthritis is caused by infectious agents (bacterial, viral, mycobacterial, and fungal), which enter into the joint either through blood, or open wound. It is usually mono arthritis, and affects mostly the knee, hip, shoulder, wrist, elbow, and finger joints. Swelling, hot, and sometimes red, the joint affected is so painful that mobility is almost impossible. In most cases, the patient has fever accompanied by chills.
Although people at any age can be affected, young children and older adults are most likely to develop septic arthritis. Once infectious arthritis is detected in an individual, the germs must be isolated immediately to avoid severe damage. Some types of septic arthritis are:
- Viral arthritis is mainly due to HIV, rubella and hepatitis virus, and parvovirus (a type of virus responsible for exanthemata suffered in some African Arbovirus and Australian). The damage usually affects a few joints and remains moderate. Viral arthritis is less painful and cured within a few days of treatment without after-effects.
- Sexually Transmitted Arthritis is a serious type of septic arthritis that includes gonococcal arthritis, arthritis of Secondary syphilis, reactive arthritis and certain arthritis caused by HIV infection.
- Tuberculosis arthritis is a rare type of infectious arthritis due to tuberculosis. It had virtually disappeared with the BCG vaccination and antibiotic treatment of TB infections. However, the number increases today because of the profound immunodeficiency induced by the AIDS virus, which makes certain nontuberculous mycobacteria, normally harmless, pathologic in those infected by HIV.
Microcrystalline arthritis – In this type of arthritis, inflammation is triggered by accumulation in the joints of microcrystal uric acid, calcium pyrophosphate (chondrocalcinosis) or Apatite disease (multiple calcium deposits in cartilage, joint fluid and tissues around joints). In this group of arthritis, the joints become swelling and transitionally very painful. Usually, the patients are recovered without after-effects.
Arthropathy – is a rare form of medical condition observed during certain diseases of the nervous system (diabetes, leprosy, Tabes dorsalis, syringomyelia, paraplegia and quadriplegia) causing a loss of sensitivity in the joints. Due to lack of pain sensation, any trauma or pressure exerted on the affected joints produce no reflex contraction to protect the muscles, but an exaggerated mobility, which could damage the joints and create a significant distortion called Charcot’s joint (A chronic, progressive and degenerative disease of one or more joints).
What is the diagnosis of arthritis?
The diagnosis of arthritis is mostly based on your medical history and physical exam to determine which joints are affected. Your doctor will seek for the presence of inflammation, pain, stiffness and other signs of arthritis. If the physical examination shows that there are more than one painful joint, your physician will recommend lab tests, x-ray examinations, and arthroscopy to confirm the diagnosis.
Blood test – Blood tests can be performed to find Rheumatoid factor (RF or RhF), an antibody indicating rheumatoid arthritis or polyarthritis. The blood test may be accompanied by urine tests and joint fluid analysis to detect presence of other types of arthritis such as gout or ankylosing arthritis.
X-rays – X-rays and magnetic resonance imaging (MRI) are often part of the diagnosis of arthritis. Your doctor may recommend these exams to detect bone spur (bony growth formed on normal bone) in the joints affected by osteoarthritis.
Arthroscopy – a medical procedure consists of inserting, by surgical intra-articular, a small, flexible camera (arthroscope) in the infected joint to detect articulatory problems: pain, swelling, nerve damage, instability, etc. The arthroscope transmits image from inside to a video screen allowing the surgeon to see any disorder in your joint. In general, this procedure has few complications.
Arthritis Treatment
Certain forms of arthritis are incurable with either drugs or physiotherapy. Arthritis for which there is no cure, treatments are aimed at reducing symptoms such as pain and inflammation. Some forms of arthritis require special treatment: antibiotics are used in the treatment of septic arthritis; Uricosuric medications can be prescribe to treat gout; and anti-inflammatory corticosteroids are used against rheumatoid arthritis.
In most types of arthritis, pain medications and anti-inflammatory drugs (aspirin, Soma, codeine, Vioxx, Ansaid, Arthrotec, Cataflam, etc.) are used to relieve the symptoms. Some aseptic inflammatory arthritis (also called inflammatory arthritis) can cause deformities or destruction of joints. In these cases, your physician can refer you to a surgeon for an arthroplasty (replacement of articulation with a prosthetic) or arthrodesis (surgical replacement of a malformed or degenerated joint by an artificial one).
The treatment of septic arthritis must start early, because the lesions of bone and cartilage resulting from germs can become irreversible within a few days. Your physician, until the germ is identified, may begin antibiotic treatment. To prevent more damage, a few days of rest with the immobilization of the affected joints may be necessary. The treatment of microcrystalline arthritis is based on the condition of the disease.
If you have arthritis, you must avoid making efforts especially during the pain; resting is one of the most effective ways to alleviate arthritis pain. In addition to rest, avoid stress, anxiety and all activities capable of causing nervous fatigue. However, breathing exercises, sleep, mental relaxation, and meditation are very helpful in preventing arthritis pain.
Arthritis Prevention
 Unlike many other diseases; you can reduce your risk of developing certain types of degenerative arthritis such as osteoarthritis. The most effective means are to live a healthy lifestyle and maintain a healthy weight. In fact, if you are diagnosed with arthritis, regardless of the type of arthritis, you can manage to reduce the pain by changing your lifestyle and using a variety of health tips.
Unlike many other diseases; you can reduce your risk of developing certain types of degenerative arthritis such as osteoarthritis. The most effective means are to live a healthy lifestyle and maintain a healthy weight. In fact, if you are diagnosed with arthritis, regardless of the type of arthritis, you can manage to reduce the pain by changing your lifestyle and using a variety of health tips.
Although these methods cannot cure arthritis, they may temporarily reduce pain and stiffness of the disease. In general, to keep arthritis under control or reduce its pain you can:
- Sleep 7-8 hours per night
- Do exercise regularly
- Do less aggressive work, and rest urding the day
- Practice relaxation once many times a day
- Practice message therapy